- All
- Product Name
- Product Keyword
- Product Model
- Product Summary
- Product Description
- Multi Field Search
- Home
- About Us
- Products
- Customer Services
- MEDICAL INFOR
- Contact Us
Views: 0 Author: Site Editor Publish Time: 2025-11-07 Origin: Site








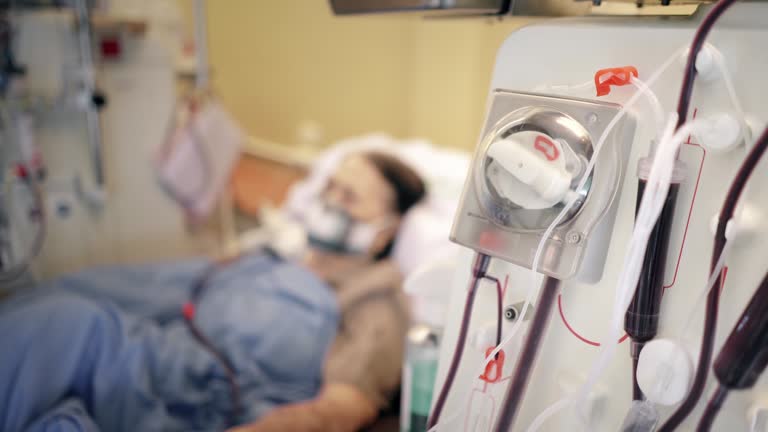
The dialyzer (also known as a dialyzer filter) is the most critical component in a hemodialysis system. It functions as the “artificial kidney,” responsible for safely and effectively removing metabolic waste products (such as urea and creatinine) and excess fluid from the blood. Its performance directly determines the outcome of the entire dialysis process.
· Filtration Core: Inside the dialyzer are thousands of extremely fine hollow fibers (the dialysis membrane). Blood flows inside these fibers, while dialysate flows around them on the outside. Waste products and water pass through microscopic pores in the membrane by diffusion and ultrafiltration.
· Direct Impact on Results: The key performance parameters of a dialyzer—including its dialysis efficiency (the rate and extent of solute clearance), water removal capacity, and ability to retain essential proteins (such as albumin)—determine whether each treatment can achieve the expected therapeutic outcome.
· Material Differences: Mainstream hemodialysis membranes are made of biocompatible synthetic polymers (such as polysulfone and polyethersulfone) or modified cellulose materials. Synthetic membranes, due to their excellent and stable performance, continue to dominate the market.
· Performance Preferences:
*Europe: Preference for high flux polysulfone dialyzers, which demonstrate superior clearance of middle- and large-molecule toxins.
*United States: Focus on efficiency and overall performance; high-performance synthetic membranes (such as polyethersulfone) are widely used.
*Emerging Markets: Maintain steady demand for cost-effective and reliable cellulose and modified cellulose membranes.
In Summary: Selecting a dialyzer filter that matches clinical requirements begins with understanding the characteristics of its membrane material (e.g., flux level) and the key design performance indicators (clearance efficiency, ultrafiltration capacity, and protein retention). These factors form the scientific foundation that ensures the effective operation of the “artificial kidney” in extracorporeal blood purification.

Dialyzers are primarily classified according to two key parameters: ultrafiltration capacity (low flux vs. high flux) and membrane material (cellulose vs. synthetic). These two dimensions determine their clinical applications and therapeutic performance.
Dialyzers are categorized based on their ability to remove fluid and solutes—known as flux capacity:
· Characteristics: Constructed with denser membranes, allowing smaller amounts of fluid and solute to pass through per unit time.
· Main Clearance Capability: Primarily effective in removing small-molecule toxins such as urea and creatinine.
· Typical Applications: Used in basic dialysis treatments or for patients requiring high stability (e.g., those with cardiovascular instability).
· Advantages: Stable operation and relatively lower cost.
· Characteristics: Feature larger pore sizes and a higher Ultrafiltration Rate (UFR), enabling superior permeability for both water and solutes.
· Main Clearance Capability: Remove not only small molecules but also effectively eliminate key middle-molecule toxins such as β2-microglobulin, which, if accumulated, increase long-term health risks.
· Advantages: Provide more efficient and comfortable dialysis treatment, reducing post-dialysis fatigue or discomfort.
· Note: High flux dialyzers require ultrapure dialysate to prevent backfiltration of contaminants.
· Key Insight: The main advantage of high flux dialyzers lies in their broader toxin removal spectrum and enhanced regulation of middle- and large-molecule balance within the body.
The membrane material determines the dialyzer’s biocompatibility, clearance performance, and long-term stability.
· Source: Derived from natural cellulose materials such as regenerated cellulose.
· Characteristics: Cost-effective and still used in certain markets.
· Limitations: Natural cellulose materials tend to have lower biocompatibility; blood contact may trigger mild inflammatory reactions in some patients. Their flux is usually lower, commonly used in low-flux dialyzers.
· Common Materials: Polysulfone (PS), Polyethersulfone (PES), and Polymethylmethacrylate (PMMA).
· Characteristics:
*Excellent biocompatibility, minimizing blood–membrane reactions and reducing inflammation risks.
*Precisely controlled pore size distribution and stable structure, enabling the production of various flux ranges from low to very high.
*Outstanding mechanical and chemical stability, allowing compatibility with multiple sterilization methods and transportation conditions.
· Industry Position: Due to their superior overall performance, synthetic membranes have become the global mainstream choice in modern dialysis therapy.
The performance of a dialyzer filter is determined by its core technical parameters. Understanding the following four key indicators is essential for effective product comparison, procurement decisions, and clinical adaptation.
This parameter reflects the rate at which the dialyzer removes water per unit of transmembrane pressure (unit: mL/h/mmHg).
· Higher UFR → Greater fluid removal efficiency in the same amount of time (suitable for patients requiring rapid fluid removal).
· Lower UFR → Prolonged dehydration time, possibly resulting in incomplete target ultrafiltration.
Selection Guideline: UFR must be matched with the patient’s target fluid removal needs and the dialysis machine’s pressure control accuracy. High UFR dialyzers require precise ultrafiltration management systems for safe operation.
KoA represents the efficiency with which a dialyzer removes small-molecule toxins such as urea and creatinine (unit: mL/min). The higher the KoA, the better the small-molecule clearance capability.
· High KoA (>600): Enables efficient toxin removal within a shorter treatment time or at lower blood flow rates.
· Low KoA (<500): Requires longer sessions or higher blood flow rates to achieve similar clearance.
Selection Guideline: KoA is directly related to treatment duration and the patient’s vascular condition (i.e., attainable blood flow rates).
This metric quantifies the dialyzer’s ability to remove middle-molecule toxins such as β2-microglobulin (unit: mL/min). Accumulation of this substance may lead to joint disorders and tissue damage.
· High Clearance (>40 mL/min): A defining advantage of high flux dialyzers, helping prevent complications caused by middle-molecule toxin accumulation.
· Low or No Clearance: Indicates a low-flux dialyzer with limited small-molecule clearance only.
Selection Guideline: To prevent long-term complications, dialyzers with adequate β2-microglobulin clearance should be prioritized—typically high-performance synthetic membrane high flux dialyzers.
Membrane permeability defines how easily molecules of various sizes can pass through the membrane. It ultimately determines the limits of UFR, KoA, and β2-microglobulin clearance.
· Low-Permeability Membranes: Best suited for small-molecule clearance in low-flux dialyzers.
· High-Permeability Membranes: Designed for removing both small and middle/large molecules in high flux dialyzers.
Selection Guideline: Synthetic membranes, through precise structural engineering, can be manufactured with tailored permeability—from low to very high—allowing clinicians to match dialyzers precisely to patient needs.
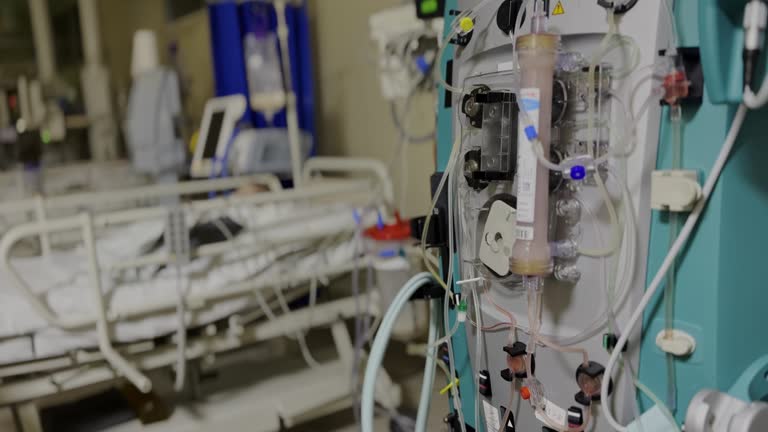
The core functionality and clinical value of a dialyzer filter depend directly on its membrane material and the innovative structural and surface modification technologies applied. High-performance synthetic membranes have become the mainstream choice worldwide, but each material offers distinct characteristics and application advantages.
Material Type | Key Properties | Primary Advantages | Typical Applications |
Polysulfone (PSU) | High structural stability, strong mechanical strength, and excellent biocompatibility | Outstanding durability, mature production process, high cost-performance balance | Widely used, especially in high flux dialyzers |
Polyethersulfone (PES) | Higher permeability and solute transfer rate, low protein adsorption | Superior toxin and fluid removal capacity, self-cleaning effect during treatment | Commonly used for high-efficiency dialysis, suitable for patients with high toxin loads or shorter treatment time requirements |
Polymethylmethacrylate (PMMA) | Unique protein adsorption capability | Actively adsorbs β2-microglobulin and other middle-molecule toxins; helps reduce inflammatory reactions | Used in specific cases—patients with elevated β2-MG or persistent inflammatory responses |
-Structural Concept:
Thousands of hair-thin hollow fibers (approximately 200 microns in internal diameter) are densely packed within the dialyzer housing.
-High Surface Area-to-Volume Ratio:
This configuration provides an exceptionally large membrane contact surface (mass transfer area) within a compact space—forming the foundation for high KoA values and overall clearance efficiency.
-Optimized Flow Dynamics:
The inner (blood) and outer (dialysate) counter-current flow design achieves the ideal balance between diffusion and convection, ensuring optimal solute removal.
Surface modification can be viewed as the “fine-tuning” or “precision finishing” of the membrane, greatly improving its clinical performance and long-term reliability.
-Hydrophilic Modification
· Reduces the membrane’s natural hydrophobicity, improving initial wetting performance.
· Minimizes clotting risk at treatment initiation; facilitates quicker and safer priming and air removal procedures.
-Biocompatibility Enhancement (Coating or Blending)
· Creates a passivated interface that mimics human vascular endothelium.
· Incorporates biocompatible molecular chains (e.g., PVP) or bioactive coatings (e.g., vitamin E derivatives).
· Significantly reduces complement activation and leukocyte stimulation, thereby decreasing chronic inflammatory responses and improving patient tolerance.
-Anti-Fouling / Nano-Bionic Surface Technology
· Constructs ultra-smooth or energy-barrier surfaces at the molecular level.
· Maintains long-term membrane permeability (ensuring stable toxin clearance throughout treatment). Lowers coagulation risk—particularly effective for PES-based membranes that benefit from this nanotechnological enhancement.
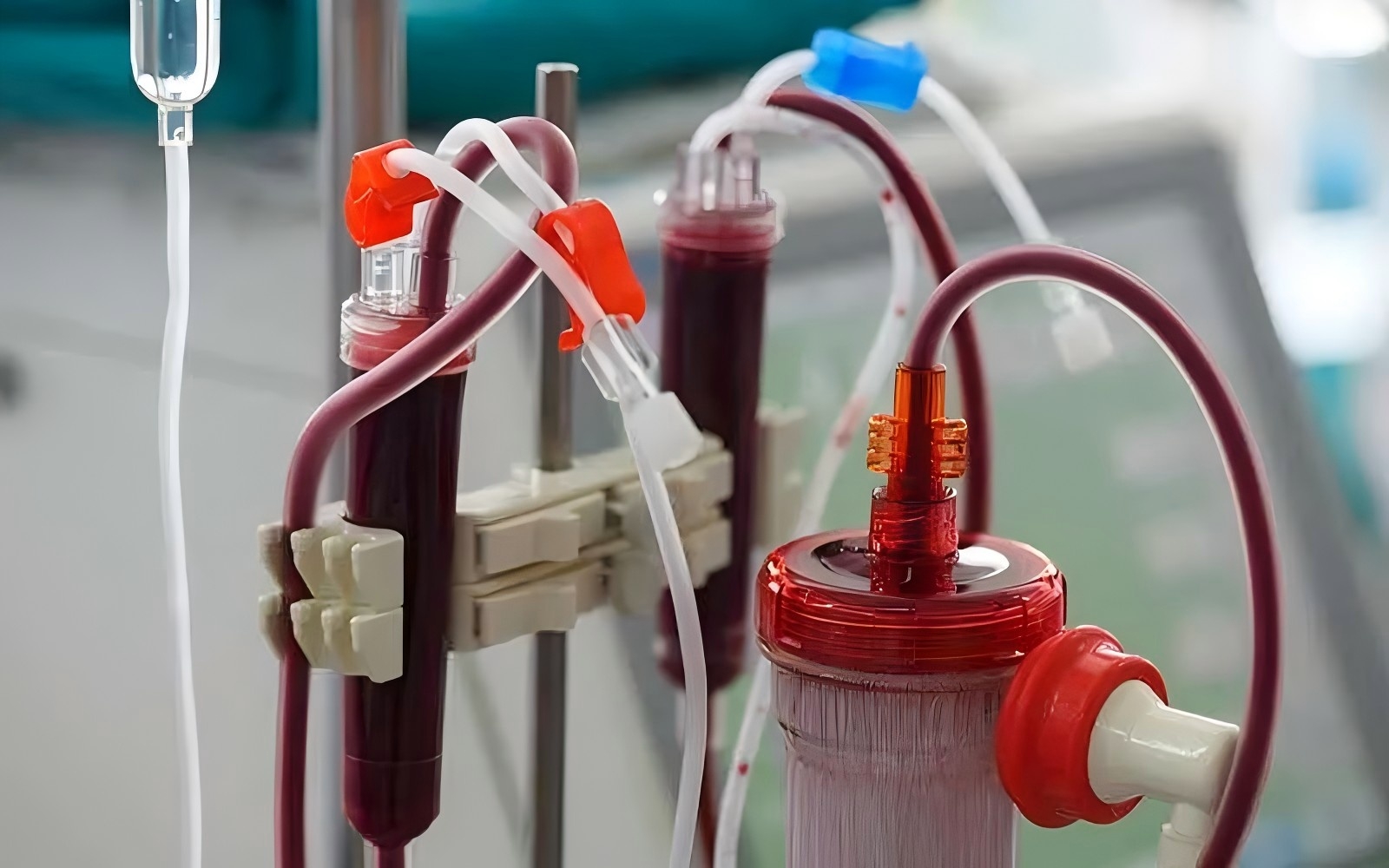
The safety and functional reliability of a dialyzer filter depend heavily on the strict sterilization methods and quality control systems applied during manufacturing. Although these processes take place behind the scenes, they are fundamental to ensuring patient safety and consistent treatment efficacy.
EO sterilization is widely used and cost-effective. However, it requires a rigorous degassing process to completely remove chemical residues. Any residual EO can be toxic, so complete elimination is essential to achieve the final level of biocompatibility and patient safety.
This method uses high-energy gamma rays for physical sterilization, eliminating microorganisms without leaving any chemical residue.
Gamma sterilization provides greater process stability and control, making it ideal for high-end dialyzers with advanced biocompatibility requirements and precise synthetic membrane structures (such as polysulfone and polyethersulfone dialyzers).
Each batch of dialyzers must undergo a series of strict verification tests to ensure both performance and safety:
· Membrane Integrity Test: Confirms there are no leaks or structural defects—this is a critical safety threshold.
· Fluid Flux and Clearance Reverification: Ensures that the actual UFR, KoA, and β2-microglobulin clearance meet the specified performance ratings, guaranteeing the dialyzer’s expected efficiency.
· Biocompatibility and Cytotoxicity Screening: Evaluates the safety of the membrane and overall materials when in contact with human blood, ensuring the product meets clinical health standards.
Choosing manufacturers certified under ISO 13485 (Medical Device Quality Management System), CE (European Conformity), and FDA (U.S. Food and Drug Administration) standards indicates that:
· The production environment and manufacturing processes fully comply with international medical safety regulations.
· The manufacturer has the capability and responsibility to continuously supply compliant, consistent, and reliable products.
· There are traceable and auditable management systems in place for raw material sourcing (e.g., membrane polymers), sterilization validation, and biological testing.
Selecting a dialyzer is not a simple product comparison—it is a systematic process of matching the patient’s physiological status, therapeutic goals, and device performance parameters. Choosing the “right” dialyzer filter for each patient is critical to ensuring both clinical efficacy and medical safety, while optimizing healthcare resources.
Selection Dimension | Key Considerations and Logic | Related Product Features |
Physiological Parameters | Body weight / body size: Determines toxin distribution volume and base fluid removal requirement; typically requires a dialyzer with high UFR and medium-to-high KoA values. Residual kidney function: Patients with partial residual renal function may require lower small-molecule clearance (KoA value can be moderately reduced). | UFR, KoA parameter matching |
Pathological Condition | Protein or nutritional status: For hypoalbuminemic patients, high flux dialyzers must be used cautiously to avoid excessive protein loss.- Presence of middle-molecule toxin accumulation (β2-MG↑) or chronic inflammation → High flux dialyzers with β2-microglobulin clearance >40 mL/min (e.g., PES or high-performance PS) are mandatory. High bleeding risk / coagulation disorders: Prefer dialyzers with hydrophilic surface modification and superior biocompatibility (e.g., modified PES or PS membranes). | Membrane material, biocompatibility, β2-MG clearance |
Prescription Settings | Dialysis duration and frequency: Short-duration dialysis (<4 hours) requires high KoA and high UFR dialyzers for time efficiency. Patients with limited blood flow (poor vascular access): A dialyzer with a high KoA can maintain clearance even at lower flow rates. | Prioritization of UFR and KoA parameters |
Patient Group / Clinical Scenario | Selection Logic | Typical Representative Options |
Conventional Maintenance Hemodialysis (No Major Complications) | Cost-Performance Strategy: Meet baseline KoA (~500 mL/min) and stable UFR requirements.Recommended: Polysulfone dialyzer (medium/high flux) with standard hydrophilic surface modification — combining safety, reliability, and economic efficiency. | PS-based standard models(e.g., B. Braun / Fresenius standard PS series) |
Patients Requiring Enhanced Middle-Molecule Clearance / Inflammatory Control | Performance Priority Strategy: β2-microglobulin clearance >45 mL/min. Recommended: High flux PES dialyzer with anti-protein-adsorption surface modification — effectively prevents amyloidosis and inflammation-related complications. | PES flagship models(e.g., Baxter / Asahi high-end PES series) |
High-Risk or Special Pathophysiological Conditions | Customized Strategy: - Hypoproteinemia: Avoid ultra-high flux membranes; select moderate-flux PS/PES dialyzers with nutritional monitoring. - Refractory β2-MG accumulation or inflammation (e.g., dialysis-related amyloidosis): Consider PMMA adsorptive membranes. | PMMA specialized models(e.g., Toray customized therapy units)Mid-flux PS with anticoagulation optimization(e.g., NIPRO safety-priority products) |
Short-Term High-Efficiency Dialysis Requirement | High-Performance Strategy: Must combine high KoA (>700 mL/min), high UFR, and high flux membranes.Hospital systems must ensure accurate blood flow and fluid control capabilities. | Triple-high models (High KoA / UFR / β2-MG)(e.g., Fresenius 600S series) |
As the core component of blood purification, the dialyzer directly determines both the treatment safety and quality of life for patients undergoing hemodialysis. The precision and stability of its technology define the overall reliability of the entire dialysis system.
In the context of global healthcare, where demand for high-performance, customizable, and reliably supplied dialysis products continues to grow, choosing a partner with advanced technical capability and a rigorous quality control system is essential.
CN MEDITECH Dialyzer Series is built on a foundation of advanced membrane technologies— including modified polyethersulfone (PES) membranes, anti-protein-adsorption surface coatings, gamma irradiation sterilization, and a comprehensive ISO 13485 / FDA-compliant quality system—to deliver the following key advantages for global distributors and healthcare institutions:
✅ Modular Dialyzer Solutions – Covering the full range from standard to ultra-high flux dialyzers.
✅ Professional ODM / OEM Support – Tailored to regional clinical needs and technical standards.
✅ Traceable, Zero-Compromise Medical Safety Assurance – Ensuring each dialyzer filter meets the highest global regulatory and performance benchmarks.
content is empty!